Medicaid is an important source of healthcare coverage for millions of people in the United States. But does it cover the cost of keloid removal? In this article, we’ll explore the specifics of Medicaid coverage for keloid removal, so you can make an informed decision about your healthcare options.
Contents
Does Medicaid Provide Coverage for Keloid Removal?
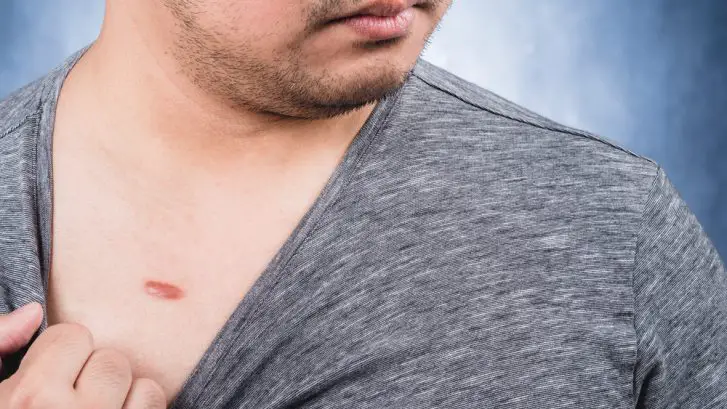
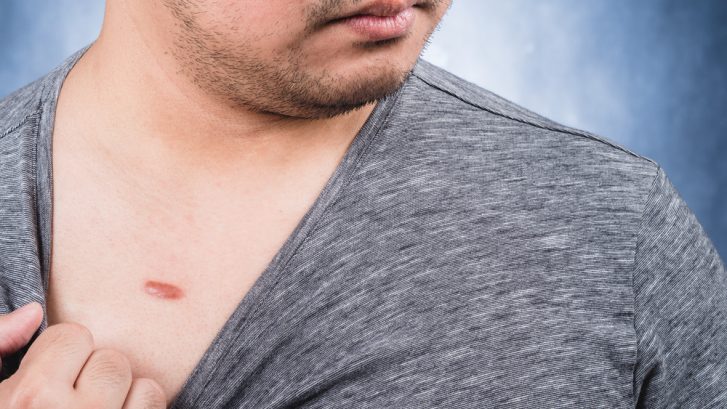
Keloids are raised, fibrous growths that develop in the skin after a wound has healed. They can be caused by cuts, scratches, burns, or even piercings. Keloids can also be painful and itchy, and cause emotional distress. Since keloids are not typically dangerous, most health insurance companies do not cover the cost of their removal. However, Medicaid covers some treatments for keloids, so it is worth exploring if you have this type of insurance.
What is Keloid Removal?
Keloid removal is a procedure used to remove any raised scar tissue or fibrous growths that form on the skin. This is usually done with a combination of surgery and other treatments such as cryotherapy, laser treatments, and corticosteroid injections. The goal of the procedure is to reduce the size and appearance of the keloid, as well as reduce any itching or pain associated with it.
Does Medicaid Cover the Cost of Keloid Removal?
Medicaid is a government-funded health insurance program for low-income individuals and families. Each state has its own Medicaid program, so the coverage for keloid removal can vary from state to state. However, most states will cover the cost of keloid removal if it is deemed medically necessary. In some cases, Medicaid will also cover the cost of other treatments, such as laser treatments, to reduce the size and appearance of the keloid.
What is the Process for Obtaining Coverage?
The process for obtaining coverage for keloid removal is relatively simple. First, you must contact your Medicaid provider to see if they cover the cost of keloid removal. If they do, they will provide you with a list of approved providers and will help you to schedule an appointment. At the appointment, your provider will evaluate your keloid and decide if it is medically necessary to remove it. If it is determined to be medically necessary, Medicaid will cover the cost of the procedure.
Are There Any Restrictions on Coverage?
Yes, there are some restrictions on the coverage for keloid removal. Most Medicaid programs will only cover the cost of the procedure if it is deemed medically necessary. In addition, some Medicaid programs may have age or income restrictions, so it is important to check with your provider to see if you qualify for coverage.
What is the Cost of Keloid Removal?
The cost of keloid removal can vary depending on the size and location of the keloid, as well as the type of treatment used. The average cost of keloid removal ranges from $500-$3000. If you have Medicaid, the cost of the procedure may be covered, but it is important to check with your provider to make sure.
Conclusion
Keloids are raised, fibrous growths that develop in the skin after a wound has healed. Most health insurance companies do not cover the cost of their removal, but Medicaid may provide coverage, depending on your state and the type of treatment used. It is important to contact your Medicaid provider to see if you qualify for coverage and to determine the cost of the procedure.
Related Faq
Does Medicaid Cover Keloid Removal?
Answer: Yes, Medicaid does cover keloid removal in some cases. Generally, Medicaid will cover the removal of a keloid if it is considered a medical necessity. For instance, if a keloid is causing pain, itchiness, or other discomfort, Medicaid may cover its removal. Additionally, if the keloid is interfering with the normal function of an organ or body part, it may also be covered. In some cases, Medicaid may also cover removal of a keloid for cosmetic purposes. It is important to note that Medicaid does not cover all types of keloid removal procedures and coverage for specific procedures may vary by state.
What Are the Different Types of Keloid Removal Procedures?
Answer: There are several different types of keloid removal procedures that may be covered by Medicaid. These include cryosurgery, laser surgery, steroid injections, and surgical excision. Cryosurgery involves freezing the keloid with liquid nitrogen, while laser surgery uses high-energy light to remove the keloid. Steroid injections can reduce the size of the keloid and its associated symptoms, while surgical excision involves cutting it away with a scalpel. Each of these procedures is typically done under local anesthesia and may require multiple treatments to achieve desired results.
What Is the Success Rate of Keloid Removal Procedures?
Answer: The success rate of keloid removal procedures vary depending on the type of procedure and the size and location of the keloid. Cryosurgery and laser surgery typically have success rates of around 50-75%, although results may vary from person to person. Steroid injections can reduce the size of a keloid, but may not completely remove it. Surgical excision has the highest success rate of around 85-90%, but may also result in scarring.
Are There Any Risks or Side Effects Associated With Keloid Removal?
Answer: Yes, there are some risks and side effects associated with keloid removal procedures. These include infection, scarring, and recurrence of the keloid. Additionally, there is a risk of nerve damage, changes in skin color, and pain associated with some of the procedures. It is important to discuss these risks with your healthcare provider before undergoing any keloid removal procedure.
What Are Some Non-Invasive Treatments for Keloid Removal?
Answer: In addition to the surgical procedures covered by Medicaid, there are also some non-invasive treatments for keloid removal. These include silicone gel, laser therapy, and topical medications. Silicone gel is applied directly to the keloid and can reduce inflammation, itchiness, and pain. Laser therapy is used to reduce the size of the keloid, while topical medications can help to reduce swelling and redness. It is important to note, however, that these treatments may not completely remove a keloid.
How Long Does It Take to Recover From Keloid Removal?
Answer: The amount of time it takes to recover from keloid removal depends on the type of procedure and the size and location of the keloid. Generally, cryosurgery and laser surgery require a recovery period of a few days to a few weeks. Steroid injections may require a few weeks to a few months, while surgical excision may require up to 6 weeks of recovery time. It is important to follow your healthcare provider’s instructions to ensure proper healing.
As a professional writer, it can be concluded that Medicaid does provide coverage for keloid removal. Depending on the state, the Medicaid program may provide coverage for the removal of keloids through a variety of methods, including surgery, laser therapy, cryotherapy, radiation therapy, and corticosteroid injections. However, the coverage may vary from state to state, and patients should consult their local Medicaid office to determine coverage options available in their area. Furthermore, many private health insurance policies may also provide coverage for keloid removal.